Colorado’s five largest health insurers would have to pay $40 million in new fees next year — fees that will be passed along to customers — to keep afloat an enterprise subsidizing certain insurance costs, under a bill that passed from its first Senate committee Thursday.
Senate Bill 178, sponsored by Democratic Sens. Kyle Mullica of Thornton and Iman Jodeh of Aurora, would offer a short-term injection to the soon-to-be-insolvent Health Insurance Affordability Enterprise through a combination of the fees and $100 million in bond sales. Supporters acknowledged it is a temporary fix when a long-term solution is needed for the enterprise that includes the state’s reinsurance, OmniSalud and state-exchange subsidies programs, but they said something must be done immediately.
The program, which has been impacted by federal funding reductions over the past year-plus, faces a $139 million chasm between its funding and projected spending in 2027, Colorado Insurance Commissioner Michael Conway told the HIAE board in January. While critics like Republican Sen. Barbara Kirkmeyer attribute the shortfall to overspending — and an audit of the enterprise is due to be completed by early next year — Jodeh warned that 40,000 people could lose insurance next year without this funding.
“We heard several times from both sides the question of ‘Why?’ The simple answer is that these are people, and they matter — and their being able to have access to healthcare matters,” Mullica, a hospital nurse, told the Senate Finance Committee on Thursday. “If we don’t pass a bill, there are real impacts on real people in our communities.”
Could passage of the bill also people getting policies from health insurers?
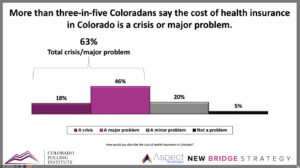
A slide from a media presentation shows the concerns about health-insurance costs that the Colorado Polling Institute recorded in late 2025.
But insurers warned the bill could have the unintended impacts of raising insurance costs enough that people, particularly those on the individual market, will forego insurance next year and be without coverage at the expense of people aided by the fee.
SB 178 splits the $40 million fee evenly between the five largest insurers — Aetna, Anthem Blue Cross Blue Shield, Cigna, Kaiser Permanente and United Healthcare — but the impacts on their customers vary wildly. Aetna, for example, is the smallest of the five by a significant factor and will have to increase per-member monthly costs by $40.40 — about $480 a year — while its competitors will have to charge no more than about $5 a month to cover the costs, officials said.
“I can’t compete if I enter the market at a 35 dollar per-member per-month deficit,” said Marc Reece, executive director for public policy for CVS Health, which owns Aetna.
SB 178 marks the second straight year that legislators have had to scramble to find funding for the HIAE, which already charges fees of 2.1% on each for-profit health-insurance policy sold in the state and 1.15% for each nonprofit policy. Legislators planned to seek authorization for a fee hike during the 2025 special session, but Mullica, fearing the effect of increased fees on already cost-racked Coloradans, stepped in and changed the bill so that legislators could get $100 million for the enterprise by selling tax credits instead.
Why sponsors went this route with health insurers
This year, however, options were more limited, and Mullica said he wanted the industry to pay for a portion of the $140 million in costs to get their buy-in on the program. The $100 million in bonds will be repaid over a period not exceeding 45 years with the fees already coming into the HIAE — an annual cost that Mullica estimated around $10 million that will be used for that purpose rather than funding insurance costs.
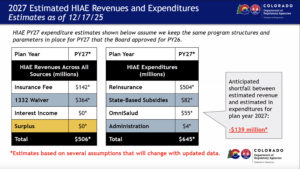

A slide from the January meeting of the Health Insurance Affordability Enterprise board meeting explains the expected funding shortfall for the HIAE next year.
The fund’s biggest expense — an expected $504 million next year — is a reinsurance program that lets insurers dip into a fee-funded pool to pay for the highest-cost cases and, in doing so, allows them to keep down individual-market premiums in high-cost areas like the mountains and Western Slope where limited doctors demand higher reimbursements. Much of that program’s funding — $364 million — comes from a federal waiver based on the amount of money that program is estimated to save people.
But the $82 million needed for state-based subsidies for lower-income Coloradans buying individual and family insurance through the Connect for Health Colorado exchange and the $55 million for OmniSalud come from the existing fee, expected to raise $142 million in 2027. OmniSalud is a Colorado program that funds premium-free insurance policies for undocumented immigrants of limited income who don’t qualify for Medicaid.
HIAE programs already have taken cuts
The shortage of funding reduced OmniSalud from 12,000 slots in 2025 to 6,700 this year, but critics like Kirkmeyer have said that recipients should have to pay at least some minimal premiums as most of those helped by other HIAE programs do. While OmniSalud participants don’t pay premiums, program supporters said they are willing to discuss that change if it can get more people covered, and the changes this year raised their co-pays and deductibles, noted Christina Walker, senior director of policy for Healthier Colorado.

Colorado state Sen. Barbara Kirkmeyer airs her concerns about Senate Bill 178 on Thursday.
Beyond raising costs for insured Coloradans while the state is becoming increasingly expensive to live in, SB 178 also violates the Taxpayer’s Bill of Rights, said Trey Rogers, an attorney at Recht Kornfeld and general counsel for former Gov. Bill Ritter.
Fees that fund enterprises must offer a commensurate service to those entities who pay them, Rogers told committee members. But it’s only Coloradans on the individual insurance market and the companies that provide them policies that will benefit from this proposal. And some insurers who will pay the fee — including Aetna and Cigna, which announced Thursday that it is pulling out of the individual market nationwide — will get nothing from what they pay, he said.
In fact, the purpose of the HIAE — to provide stability to the health-insurance market, as Conway described on Thursday — is not a tangible benefit that could qualify as TABOR-allowable, Rogers said. Therefore, if someone were to sue over the legality of this new fee, a court could find the enterprise to be unconstitutional and cut off funding to all three of the programs it oversees.
“No Colorado court has held that it’s permissible for Colorado to collect a fee from a payer who won’t see benefits from the program,” Rogers said.
Backers defend proposal
Conway pushed back, saying that all insurers benefit from the program. By getting more Coloradans who otherwise couldn’t afford to purchase health insurance covered, the HIAE increases funding for healthcare providers who get little from Medicaid patients and almost nothing from uninsured patients, he explained. And by doing that, providers don’t shift costs by way of higher prices to commercially insured patients, which in turn would cause insurers to raise premiums on those patients.

Colorado state Sens. Marc Snyder and Adrienne Benavidez listen as Colorado Insurance Commissioner Michael Conway speaks during a committee hearing on Thursday.
Once again, the debate over healthcare costs that erupted at Thursday’s committee hearing pitted providers and insurers against each other.
Josh Hannes — vice president of rural policy and strategy for the Colorado Hospital Association, which supported SB 178 — warned that with federally based cutbacks coming to Medicaid next year, health centers anticipate a rise in uncompensated care and have to raise costs or shut down lines of service to offset that. Insurers, he said pointedly, offer no services that are uncompensated, and their premiums have grown much faster over the past decade than hospital prices.
Reece, however, said that as much as hospitals have said they can stop the cost shift if more people are insured, they have not lowered prices in recent years as programs like those offered by the HIAE have kept Coloradans covered. And he said that if hospitals had to raise costs based on a “marginal change in the individual markets,” they already would have done so.
Senators want future plan
Committee members advanced SB 178 to the Senate Appropriations Committee on a Democrat-led 6-3 party-line vote, but several did so without enthusiasm. Sen. Chris Kolker, D-Centennial, questioned why the state would incur multi-decade debt through bond sales to fund a program for one year, while Sen. Marc Snyder, D-Manitou Springs, said he wants to see a better solution come forward next year.
“This is not a pleasant experience. This is generally not a bill I support,” said Snyder, who has been critical of his party’s strategy of raising fees to fund new enterprises. “But I understand the situation, and we don’t want people out there getting cut off from health insurance … I’d say I’ll hold my nose (while voting for it), but that would be unprofessional.”
Mullica and Conway both vowed to look for new ways to fund the enterprise long-term during the off-session, but neither offered details for how that could be done on Thursday. Both warned, however, that without the continuation and potential expansion of programs like OmniSalud, more Coloradans could go uninsured and put off care until their conditions become acute, which will lead to floods of uninsured residents seeking high-cost care in emergency rooms without any means to repay it.
A short time to pass bill
Meanwhile, Kirkmeyer asked what she is supposed to tell cash-strapped residents about why they’ll pay more in insurance costs next year — hundreds of dollars more, in some cases — so that people who pay no premiums can have policies. And she warned that the new fee could spur lawsuits that put multiple programs under a court’s spotlight.
“When the payor of the fee does not benefit from the fee they are paying, that is a violation of TABOR,” she said. “I think you should strongly consider how you are jeopardizing the entire enterprise.”
SB 178 must make it through the Senate and House before the legislative session adjourns on May 13.
